Hypernatremia is a condition of excess blood sodium levels. Defined as sodium levels of more than 145 mEq / L. Severe hypernatremia is defined as plasma sodium level ≥156 mEq / L. This condition signifies the loss of the amount of water in the body. Severe acute hypernatremia is an emergency condition. In this article we will discuss the management of hypernatremia
Daftar Isi
Regulation of Sodium and Water in the Human Body
Sodium is very closely related to water in the body. The mechanism of regulating sodium and water levels in the body is closely related. Therefore, the condition of impaired blood sodium levels is related to diseases that interfere with total water levels in the body.
Although less common, hypernatremia causes 40-60% more deaths than hyponatremia. Therefore, hypernatremia needs attention especially in the emergency department.
Water Balance in the Human Body
One important aspect in understanding hypernatremia is to link it to the composition of body water. In general, total body water (TBW) covers 60% of men’s body weight and 50% of women. TBW is further divided into extracellular fluid components and intracellular compartments. Components of extracellular fluid include plasma, interstitial fluid, lymph fluid, connective tissue, bone, fluid in the body’s cavity, and fat tissue. See the picture below:

From the picture above, it is explained that sodium is the main electrolyte component of extracellular body fluids. The presence of this electrolyte is often maintained so that the viscosity or osmolality of the liquid is maintained. This is to ensure that the cell can work properly.
Hormones that Regulate Water Balance
The way the body regulates water balance is primarily to sense osmolality of fluids. In the body, osmolality is maintained in the range 280 – 295 mOsm / L. The osmolality receptor is located at the center of the osmoreceptor in the form of a neural network, the organum vasculosum of the lamina terminalis (OVLT).
In addition to OVLT, the central nerve is also equipped with osmoreseptive neurons which are widely located in the brain. Osmoreseptive neurons can be found in the subfornical organs and nucleus tractur solitarii. This tissue allows the brain to respond integrally in keeping fluid osmilality to remain within the normal range. The response of the brain in these settings is by releasing various hormones.

Below are some of the hormones that play a role in the regulation of water and affect blood sodium levels:
- Antidiuretic hormone (ADH). This hormone is the main hormone that regulates sodium concentration. ADH secretion is stimulated by plasma hyperosmolarity, decreased effective arterial volume (EAV), and angiotensin II action. ADH causes the insertion of aquaporin-2 canals in collecting ducts in the kidneys. The effect is water reabsorption and increased urine osmolality. Urine osmolality (Uosm) without ADH is 60 mOsm / L whereas with ADH is 1200 mOsm / L.
- Aldosteon. This hormone regulates the total amount of sodium in the body. Aldosterone secretion occurs during hypovolemia (via renin and angiotensin II) or hyperkalemia (isoosmotic re-absorption of sodium in potassium or H +)
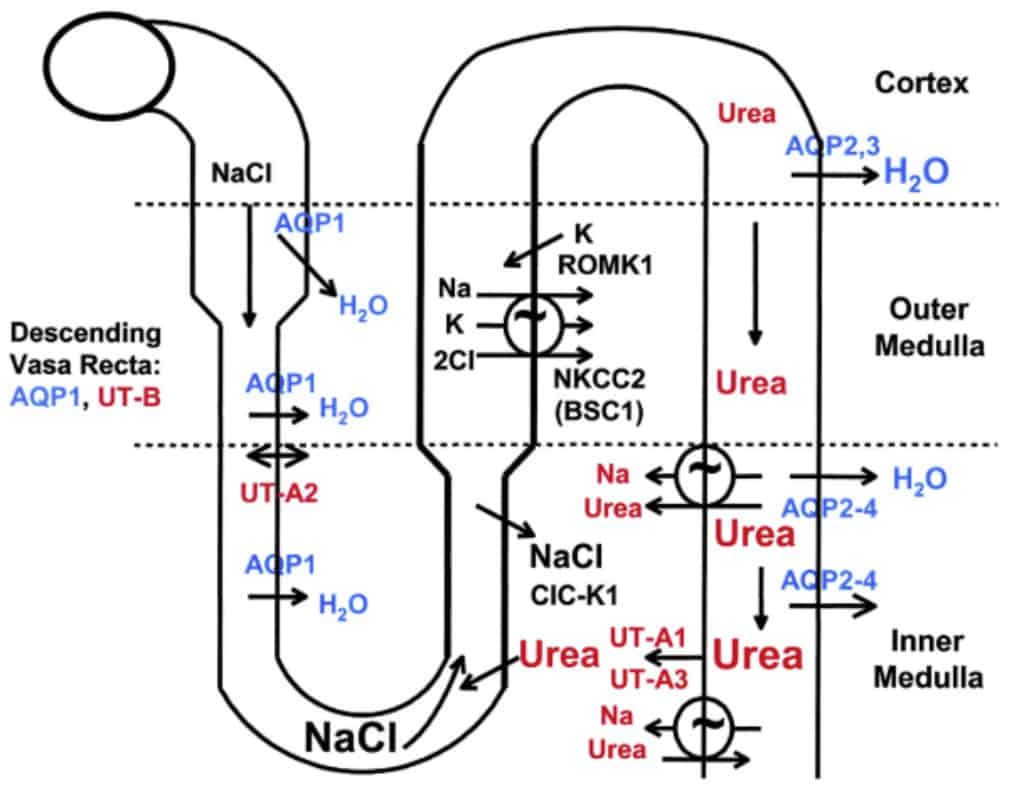
Pathophysiology of Hypernatremia
Hypernatremia occurs in conditions of a water deficit relative to the amount of sodium. Therefore, all hypernatremia patients have hypertonicity.
The condition occurs due to loss of hypotonic fluid due to dehydration or hypertonic fluid infusion. In addition, it can also be caused by a disturbance in water intake, for example in conditions of intubation, multiple sclerosis (MS), and old age. In healthy people, hypernatremia causes a strong thirst so hypernatremia usually occurs when the patient cannot drink.
Etiology or Causes of Hypernatremia
- Extrarenal water loss (Uosm >700-800 mOsm/L)
- Gastrointestinal tract: vomiting, nasogastric drainage (NGT), osmotic diarrhea, fistula
- Insensible loss: fever, activity sweating, ventilation, burns
- Loss of water in the kidneys (Uosm <700-800 mOsm / L)
- Diuresis: osmotic (glucose, mannitol, urea), loop diuretics (eg furosemide)
- Diabetes insipidus, can be central ie ADH deficiency or resistant to ADH (nephrogenic)
- Central: hypothalamic disease or posterior pituitary disorders (congenital, trauma / surgery, tumor, infiltrative disease / IgG4), can also be idiopathic, hypoxic esophalopathy, ethanol poisoning
- Nephrogenic: congenital (ADH V2 receptor mutation, aquaporin-2 mutation), drugs (liitum, amphotericin, demeclocycline, foscarnet, cidofovir), metabolic (hypercalcemia, severe hypocalemia, protein malnutrition, congenital abnormalities), tubulointerstitial disease (positional phase) recovery of acute tubular necrosis / ATN, polycystic kidney disease, sickle cell, Sjogren, amyloidosis), pregnancy (production of vasopressinase from the placenta)
- Others (Uosm >700-800 mOsm/L)
- Sodium overload: hypertonic fluid (eg resuscitation with bicarbonate / NaHCO3 fluid), mineralocorticoid
- Seizures: an increase in intracellular osmol causes a shift in water into the cell, causing transient hypernatremia in the serum
Diagnosis of Hypernatremia
The interview aims to determine the cause of hypernatremia. A history of head trauma can be a clue to central diabetes insipidus. A history of psychiatric illness with lithium drug consumption could be the key that leads to nephrogenic DI. In addition, hypernatremia that occurs within 48 hours is classified as acute hypernatremia while the onset of more than 48 hours or unknown is categorized as chronic hypernatremia.
Acute hypernatremia usually gives more obvious symptoms than chronic conditions. These symptoms can be lethargy, weakness, irritability, and if severe can be a seizure or coma.
In acute conditions, the brain can shrink due to the shift of water from brain tissue to plasma fluid. In this condition, it can cause brain volume to shrink and can cause rupture of blood vessels causing subarachnoid bleeding and / or subdural hematoma. However, bleeding complications generally occur in infants or pediatric patients compared to adults.
Hyperosmosis can also cause damage to muscle tissue. If this happens, it is referred to as hypernatremia rhabdomiolysis. Due to the chronic conditions changes in electrolyte composition are more gradual, this is followed by gradual changes in electrolyte levels in the intracellular compartment so that the symptoms of chronic hypernatremia become less promising than the acute condition.
Untuk menilai adanya hipernatremia serta penyebabnya, dilakukan pemeriksaan osmolalitas urin (Uosm), natrium urin (UNa), status volume cairan tubuh (tanda vital, ortostastik, tekanan vena jugular, turgor kulit, BUN, kreatinin). Kemudian untuk menentukan penyebab, dapat mengikuti alur di bawah ini:
To assess the presence of hypernatremia and its causes, urine osmolality (Uosm), urine sodium (UNa), body fluid volume status (vital signs, orthostastic, jugular venous pressure, skin turgor, BUN, creatinine) are performed. Then to determine the cause, can follow the flow below:

Management of Hypernatremia
For treatment of hypernatremia including the improvement of access to water or meeting daily water needs (≥1 L / day or usually 30-35 mL / kg / day) and replacing the water deficit along with the fluid volume deficit. After the liquid volume has been repaired, the next step is to calculate the water deficit and the amount of the replacement fluid. Consider the equation below:
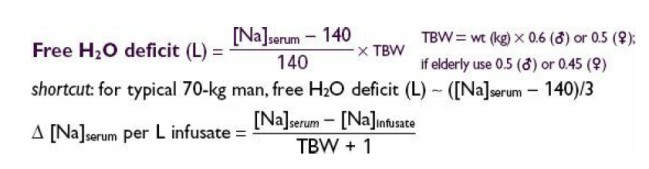
For example, if we will provide a replacement fluid in the form of 5% dextrose (D5W). So for every liter of D5W that we give to men weighing 70 kg and body sodium 160 mEq / L will reduce sodium levels around 3.7 mEq (D5W does not contain sodium).
Keep in mind that serum sodium intake should not be too fast, a maximum of 0.5 mEq / L per hour or 12 mEq / L per day and recommended only 10 mEq / L per day. If it is too fast it can cause brain edema. For example, in men weighing 70 kg, giving 125 mL of pure water per hour will reduce sodium levels 0.5 mEq / L per hour. So that the provision of water for these patients is a maximum of 125 mL per hour.
The target sodium content to be achieved is 145 mEq / L. The substitute infusion fluid that is given is various. It can be D5W or D5 ½ NS (sodium 77 mEq / L) or D5 ¼ NS (sodium 38 mEq / L). For D5 ½ NS it can provide a volume of free water of about 500 mL per liter infusat while D5 ¼ NS 750 mL free water per liter infusat. Besides being in the form of infusion, both of these liquids can also be drunk or via NGT.
To facilitate calculations, we can use a medical calculator to calculate fluid administration for hypernatremia at this link. As for the management algorithm, you can follow the flow of management below:

Special Management of Hypernatremia
If the cause of hypernatremia is due to diabetes insipidus, in the case of central DI, desmopressin (dDAVP) can be given. If the cause is nephrogenic DI, if possible overcome the cause, do salt intake restrictions, and give thiazide. This will cause mild volume depletion thereby reducing sodium output by the kidneys. In pregnancies that cause DI, dDAVP can be given.
Medical Reference Book
Berikut ini adalah beberapa buku teks yang dapat dipilih sebagai bahan pembelajaran khususnya di bidang ilmu dasar kedokteran dan penyakit dalam. Format dapat berupa buku teks fisik maupun e-book (aplikasi Kindle Google Play Store atau Apple Apps Store).
The following are some textbooks that can be selected as learning materials, especially in the basic fields of medicine and internal medicine. Format can be in the form of physical textbooks or e-books (the Google Play Store Kindle application or Apple Apps Store).
[adinserter block=”3″]Conclusion
Sodium is very closely related to water. The condition of hypernatremia is basically caused by a reduction in the intake of water which causes dehydration or a lot of water loss. Under normal conditions, hypernatremia rarely occurs because this condition is a very strong thirsty excitement. In the absence of access to water either in the absence of a water source or certain medical conditions, hypernatremia can easily occur.
Reference
- Adrogué HJ, Madias NE. Hypernatremia. N Engl J Med. 2000 May 18;342(20):1493–9.
- Guillaumin J, DiBartola SP. A Quick Reference on Hypernatremia. Vet Clin North Am – Small Anim Pract. 2017;47(2):209–12.
- Lindner G, Funk GC. Hypernatremia in critically ill patients. J Crit Care. 2013;28(2):216.e11-216.e20.
- Muhsin SA, Mount DB. Diagnosis and treatment of hypernatremia. Best Pract Res Clin Endocrinol Metab. 2016;30(2):189–203.
- Sabatine MS, editor. Pocket medicine. 5th ed. Philadelphia: Lippincott Williams & Wilkins; 2014.

Seorang dokter, saat ini sedang menjalani pendidikan dokter spesialis penyakit dalam FKUI. Peminat berbagai topik sejarah dan astronomi.


